
ĬD8 + T cell reaction can surpass CD4 + T cell reaction with high expression of CD69, CD38, and CD44 and enhanced expression of OX40 (CD134) and OX40L (CD252) when compared to healthy subjects, the latter is one of TNFR/TNF family members which can stimulate T cells promoting sustained T cell clonal expansion and survival making it a promising target for enhancing protection against viral infection. It was explained by direct infection of T cells and macrophages through ACE2 receptor-mediated viral entry, the aggressive inflammatory release of cytokine-favored T cell exhaustion, spleen, and lymph node invasion by the virus, and lactic acidemia that might occur in sepsis and cause inhibition to lymphocyte proliferation. Lymphopenia is a laboratory feature of severity with a substantial decline in CD4 + T, CD8 + T, natural killer cells (NC), and B cell lymphocytes as the most critical characteristics of immune dysfunction in COVID-19. Severe depletion of T cells had been demonstrated during the acute stage of this illness. Neutralizing antibody response to SARS-CoV spike (S) glycoprotein is protective, including memory B cells, but it is short-lived in cured patients. 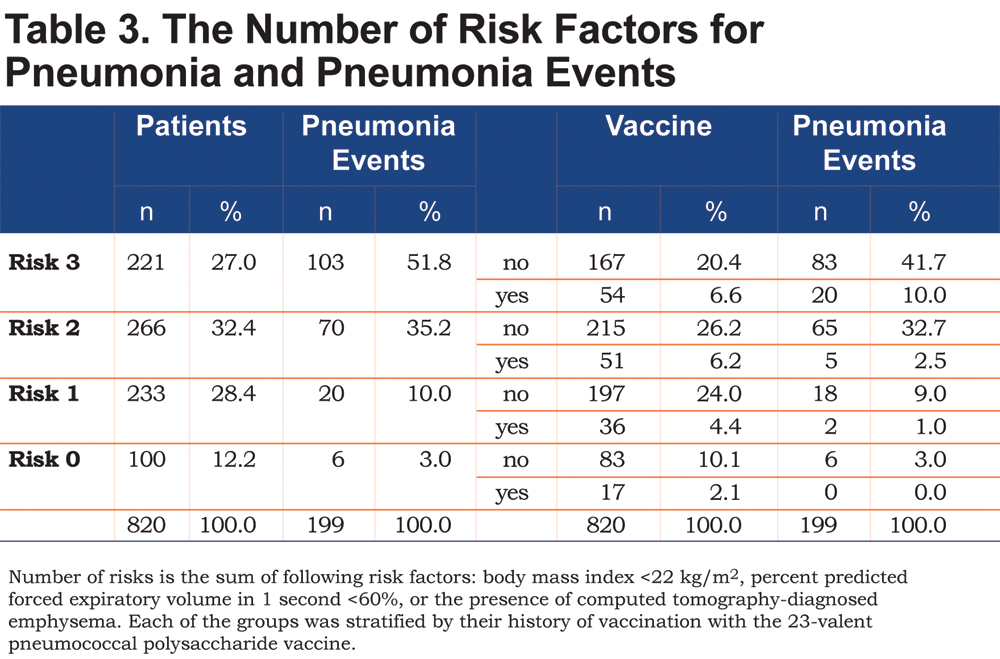
Previous experience in SARS-CoV-infected patients demonstrated a significant innate immune response as a cause of SARS-CoV-mediated disease. The potency of the vaccine is determined by disease control, which relies on the age and immunocompetence of the patient. Newly developed viral epidemics put a significant and challenging economic burden on healthcare systems. Further randomized control trials may be needed to establish a direct causation between the two and clarify these associations. The present study suggested that the combination of Prevnar13 and Vaxigrip may be related to decreased occurrence of serious respiratory infections including COVID-19. The hazard ratios of significant respiratory tract infection and death due to COVID-19 were 2.29 and 10.24 in the non-vaccinated control ( p = 0.001).The severity of COVID-19 in diabetes correlated with HBA1C ( p = 0.007), combined Vaxigrip and Prevnar13 vaccination ( p = 0.0001), serum creatinine ( p = 0.001), neutrophil–lymphocyte ratio ( p = 0.001), and thrombocytopenia ( p = 0.003). Twenty-one out of 32 (65.6%) patients in the control group had severe COVID-19. Four patients had mild COVID-19 (4%), mainly gastrointestinal with no complications. 
After Vaxigrip and Prevnar13, there is a significant improvement in respiratory symptoms and a decrease in the airflow screening questionnaire ( p = 0.0001) with a significant improvement in inflammatory parameters as neutrophil–lymphocyte ratio, ESR, CRP, and platelet count. Hundred patients with type 2 diabetes mellitus were given Vaxigrip and Prevnar13 ® vaccines and were evaluated by comprehensive clinical review, airflow screening questionnaire, and routine laboratory investigations with follow-up during the COVID-19 pandemic and compared to a control group of diabetic patients with the same inclusion criteria ( n = 100). To retrospectively assess the impact of regular yearly administration of recombinant influenza and single administration of pneumococcal conjugate vaccines on the occurrence of serious respiratory infection including COVID-19 in patients with type 2 diabetes mellitus.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
